|
End Arthritis Pain |
| "Today we Change the Practice of Medicine!" Dr. M. Oz, MD |
|
Effective Pain Management is available now - without pain medication, surgery or the need for dangerous OTC drugs |
| The Business of Pain - The Science of Suffering Collagen and Joint Disease Wrinkles and Joints Combination Approach Most Effective Treatments Wave of the Future Avazzia Pro Sport Liquid Collagen BioCell Pain Physician Document |
|
March 2014
The Business of Pain - The Science of Suffering
"Electronic Signalling Technology Will Change the Future of Medicine"
By: Dr. John Hache Chronic pain affects an estimated 116 million American adults—more than the total affected by heart disease, cancer, and diabetes combined. Pain also costs the nation up to $635 billion each year in medical treatment and lost productivity.
In late 2000, Congress declared 2001 to 2010 as the "Decade of Pain Control and Research." This attention generated research and significant evidence about effective pain assessment and management strategies.2 But this increased focus on pain assessment has not necessarily improved the management of pain in older adults. In fact Pharmaceutical Companies have taken advantage of the situation to fuel a boom in opioids that has no precedence and has left everybody with a deep concern – Was the industry trying to fill a need that was seen by physicians or did the Pharmaceutical Industry choose profits over patient safety? The fact is over the past decade as many as 100,000 Americans have died from opioid overdoses and millions have become addicted to the drugs according to Andrew Kolodny, MD, a New York psychiatrist and opioid addiction specialist who co-founded Physicians for Responsible Opioid Prescribing. The other vital question that must be answered is “are there any alternatives to the existant pain meds and narcotic drugs?
The 2010 Patient Protection and Affordable Care Act required the Department of Health and Human Services (HHS) to enlist the Institute of Medicine (IOM) in examining pain as a public health problem. Acting through the National Institutes of Health (NIH), HHS asked the IOM to assess the state of the science regarding pain research, care, and education and to make recommendations to advance the field. (Institute of Medicine of the Academies – Report Brief June 2011)
Worldwide Pain Management Market to reach 43.2 Billion Dollars by 2010 – (Global Industry Analysts.)
Opiate drugs make up the largest monetary portion of the pain management market though there is a tendency to supplement the narcotic prescription with NSAIDs to potentate the analgesic effect of narcotics such as Ibuprofen/Oxycodone. Drugs.com report that this combination may cause an increased risk of serious and sometimes fatal heart and blood vessel problems (eg, heart attack, stroke). Ibuprofen/Oxycodone may cause an increased risk of serious and sometimes fatal stomach ulcers and bleeding. Elderly patients may be at greater risk. This may occur without warning signs. In the light of this information, Physicians must refrain from following Pharmaceutical guidelines and spend the time necessary to evaluate the risks for their patients. According to the Milwaukee Journal Sentinel/Med Page today, February Issue - Prescriptions for narcotic painkillers soared so much over the last decade that by 2010 enough were being dispensed to medicate every adult in the U.S. around the clock for a month. Fuelling that surge was a network of pain organizations, doctors and Researchers that pushed for expanded use of the drugs while taking in millions of dollars from the very companies that made them, a Journal Sentinel/Med Page Today investigation found. (Nov. 1, 2011 – Every day, 40 Americans die from prescription painkiller abuse, the CDC says)
Therefore trust the Physician, and drink his remedy in silence and tranquility (The Prophet – Kalil Gibran)
So what is the State of the Science regarding pain intervention? If we look at the decade of 2001 to 2010, the Science is not good as doing more of the same thing is destined for failure at the end of the next decade as well. This will be compounded by factors such as growing consumer demand, an increase in people aged over 65 and no new miracle drugs that offer any form of cure.
The Scope of the Problem
Chronic or persistent pain is described as a personal emotional and physical experience. This pain is an unpleasant, subjective and multifaceted experience that ranges from mild discomfort to agony; the frequency may be periodic, persistent or always present. Persistent pain continues beyond the anticipated healing time of acute pain caused by injury or disease and lasts for at least 3 months and may go on for years. Incidence Persistent pain affects approximately 76 million U.S. residents - more than diabetes (23.6 million), heart disease (23.3 million) and cancer (11 million) combined.1,5,6 Older adults experience a large proportion of the persistent pain burden. More than 27 million U.S. residents, or 33% of older adults, experience pain from osteoarthritis alone.7 An estimated 25% to 50% of older adults living in the community experience significant pain at least some of the time.5 Between 44% and 80% of nursing home residents experience persistent pain.5 Breaking with Tradition Our approach to pain has been a resounding failure, as much as our fight against Cancer, Heart Disease, Diabetes and thousands of other debilitating diseases. It has not been until lately that we have started to understand our enemy. Pain itself is only a symptom of something much more furtive and sinister – inflammation. And inflammation though considered by many to be an essential part of healing may itself be totally misunderstood even though we have always understood the basic mechanism of it. Dolor Dictat . The need for pain reduction has gotten us to do and to accept some pretty silly and dangerous approaches without really comprehending the adverse and long term effects involved. Pain can control your life but traditional pharmaceutically based medical approaches can and are killing people. Pharmaceutical approaches to pain border on the fringe of patient exploitation and abuse of the powers that have been loaned to them. The liberalization of addictive opioid drugs has had some pretty serious backing over the last decade motivated by huge monetary gifts from the drug manufacturers. The following national organizations have used positions, statements, guidelines, books, and doctor education courses to set the stage for the growing use of opioid drugs in treating persistent pain. · UW Pain & Policies Studies Group - From 1999 trough 2010, got $2.5 million · American Pain Foundation - undisclosed millions from Industry including opioid. · American Academy of Pain Medicine - Last year $1.5 million from pharma for their endorsement · American Pain Society - in the last two years $1.6 million for their endorsement of opioids(16) · Federation of State Medical Boards - undisclosed amount from opioid companies for a book on opioid prescribing (1998 - book updated in 2004). By 2010 and compared to the previous year with the help of the above, pharmaceutical firms were selling four times as many prescription painkillers to pharmacies, doctor's offices and hospitals. Never in the history of medicine have so many people been exposed to so much drug. Even migraine sufferers have become a target for opioids. It is known that migraine sufferers represent approximately 10% of the American population and although Medical Science is on the verge of a cure using electronic signalling, this affliction is far from being understood by physicians. "the history of treatments for migraine is largely a story of medical "overkill" and patient exploitation" (Oliver Sacks, neurologist and author of the book Migraine.) Low Level Inflammation Of the ten leading causes of mortality in the United States, chronic, low-level inflammation contributes to the pathogenesis of at least seven. These include heart disease, cancer, chronic lower respiratory disease, stroke, Alzheimer’s disease, diabetes, and nephritis(Centers for Disease Control and Prevention 2011; Bastard et al. 2006; Cao 2011, Jha et al. 2009; Ferrucci et al. 2010; Glorieux et al. 2009; Kundu et al. 2008; Murphy 2012; Singh et al. 2011). As future studies solidify the association between inflammatory mediators and different diseases, early detection of cytokine aberrations and anti-inflammatory therapy to reduce disease risk may gain more mainstream acceptance. Medicine’s Current Anti-Inflammatory Choices NSAIDs, Steroids and Cox inhibitors have long been the anti-inflammatory medication of choice. Yet the value in promoting cure vs a long list of side effects is very controversial. It has even been found that anti-inflammatory drugs directly interfere with healing. (Reynolds JF, Noakes TD, Schweellnus MP, Windt A, Bowebank P. Non-steroidal anti-inflammatory drugs fail to enhance healing of acute hamstring injuries treated with physiotherapy S African Med J 1995: 85:517-527) Electronic Pain Relief Electricity has continuously been a powerful tool in medicine for thousands of years. All medical professionals are, to some degree, aware of electrotherapy, those who directly use electricity for treatments know of its anti-inflammatory effects. The latest technology to be introduced to the world comes as a digitally produced computer controlled sinusoidal damped electronic signal using micro current through a reflex biofeedback loop. The posted results are a long lasting anti-inflammatory effect considered to be more powerful than narcotics without the expensive, life changing dangerous side effects. “The principles of physics have been largely de-emphasized in modern medicine in favour of chemistry. These electrical treatments, a familiar application of physics, thus represent powerful and appropriate elements of physicians pain care armamentaria in the clinic and possibly for prescription for use at home to improve overall patient care and maintenance of quality of life via low-risk and potentially curative treatments.” (Pain Physician 2008; 11:6:891-907) This would correspond in essence to the comprehensive strategy put forth in a blueprint for action posted by the Institute of Medicine of the Americas dated June 2011 as Electronic Signalling devices target the point of pain and the biofeedback loop corrects the brains erroneous need to produce pain. Just this information could potentially cancel out the need for NSAID/Narcotic combinations. Many Advantages Electronic signalling better known as Biofeedback Electo Stimulation Technology is multi faceted and accomplishes many complex jobs. Because inflammation involves more than pain but also includes heat, swelling, redness and a reduction in range of motion, a proper approach would be technology that addresses all five of these well known pillars. Research on Electro Stimulation Therapy proves routine neurological, physiological and psychological benefits. Research in this field has repeatedly proven better physiological repair in far less time, while indicating absolutely no adverse reactions. Inflammation and Chronic Inflammatory Disease One of the most revealing Science based research projects in the medical field is on inflammation which seems to be the precursor to most known medical conditions that affect all biological models, animal or human. In fact it is the culprit behind almost every chronic illness. Research on type I Diabetes completed in a Toronto Ontario hospital has confirmed that inflammation is also at play in this disease. Or at least, is definitely a contributing factor until all of the information comes back to prove otherwise.
The second concept is in the fact that free electrons are able to neutralize inflammatory free radicals is based on long-standing understandings of the nature of free radicals and their involvement in inflammatory processes.
There are many scientific articles that suggest that free or mobile electrons within the body can also serve as antioxidants when they are available in sufficient quantity. That free radicals act as electrophiles attracting free or mobile electrons. That these free electrons can be delivered via micro current high voltage devices such previously described, opens a world of possibility to many people who suffer from inflammation based diseases.
Biomedical research from around the world is revealing that chronic or "silent" inflammation is the culprit behind nearly every chronic disease (Oschman, 2007). Inflammation is summarized as a localized response to trauma and infection that can wall off damaged tissues until the immune system removes foreign matter, damaged cells and/or bacteria. When the inflammatory response does not completely wind down, palpable inflammatory pockets can persist for many years, slowly releasing toxins that can damage organs anywhere in the body. The phenomenon was described by the famous stress researcher, Hans Selye (1956) in his book, "The Stress of Life" and in various articles published in the Journal of the American Medical Association (e.g. Selye, 1953) and other periodicals. A search of Pub Med revealed 1082 references to the inflammatory pouch with some specifically referring to "the Selye Pouch", for the study of inflammatory reactions (e.g. Davis et al., 1981). Selye's work tied inflammatory responses to stress, cortisol secretion and adaptation. Selye and others had obtained information that necrotic tissue breakdown products from inflammatory pockets can leak into the blood and lymphatic circulation producing slow but progressive atrophy in various organs a distance from the original site of trauma.
This inflammatory pouch concept explains how local pockets of inflammation can trigger a diversity of chronic diseases and disturbances many of which frustrate the physician because it is difficult to locate the cause. "Silent Inflammation" refers to a condition in which the inflamed site is not painful, and may go unnoticed, even though it is causing problems elsewhere in the body.
A third concept is in the fact that the human body is an informational system that uses the body's complex connective tissue to communicate information to every single cell of the body. When information loses its congruency, disease states set in.
Many questions can be answered by the above response within a new body science called the "Living Matrix", which refers to the body as a complete informational system, containing electrical and electronic componentry and terms such as conductors, resistors, capacitors and semi-conductors. This "Body Electric" responds best to electrical and electronic signaling when the right devices are used.
The successes obtained by micro current devices using high voltage to stimulate "C" fibers into producing all important molecules called "Neuropeptides" cannot be stressed enough. These devices are changing the way we are thinking in the medical world – spurred on by a silent majority that are slowly but surely gaining knowledge on how to easily solve a problem that has baffled Science since the beginning of time in spite of the pharmaceutical hype.
Testimonial
After falling down a stairway and crushing my left elbow in 1988, I have suffered with neck, back, shoulder, arm, elbow and hand pain for 23 years. I would conservatively estimate that I have taken well over 50,000 aspirin in the past 23 years. On a really good day, I would take 2 aspirin after waking up and 2 aspirin before bed time. Even though I have sometimes taken up to 24 aspirin during a really really bad day, I have refused to ever take narcotics - no matter how bad the pain.
Thanks to Biofeedback Electro Stimulation Technology, I am now "virtually" pain free. JLB – DDS
Dr. John A. Hache, DNM Professional Medical Trainer and Specialist in Micro Current Intervention
References 1. Walid MS, et al. The fifth vital sign - what does it mean? Pain Pract. 2008;8(6):417-422. 2. American Society of Anesthesiologist Task Force on Chronic Pain Management; American Society of Regional Anesthesia and Pain Medicine. Practice guidelines for chronic pain management: an updated report by the American Society of Anesthesiologists Task Force on Chronic Pain Management and the American Society of Regional Anesthesia and Pain Medicine. Anesthesiology. 2010;112(4):810-833. 3. Malanga G, Paster Z. Update on managing chronic pain in the elderly. J Fam Pract. 2007;53(12 suppl):S11-S16. 4. AGS clinical practice guidelines: the management of chronic pain in older persons. Geriatrics. 1998;53(suppl 3):S6-S7. 5. AGS Panel on Persistent Pain in Older Persons. The management of persistent pain in older persons. J Am Geriatr Soc. 2002;50(6 suppl):S205-S224. 6. American Academy of Pain Medicine. AAPM facts and figures on pain. www.painmed.org/patient/facts.html . Accessed Aug. 10, 2011. 7. Lawrence RC, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part II. Arthritis Rheum. 2008;58(1):26-35. 8. Bruckenthal P, et al. Special issues in the management of chronic pain in older adults. Pain Med. 2009;10(suppl 2):S67-S78. 9. D'Arcy Y. Pain in the older adult. Nurse Pract. 2008;33(3):18-24. 10. Schofield P, et al. Guidance for the assessment of pain in older adults: a literature review. Br J Nurs. 2008;17(14):914-918. 11. Herr K. Chronic pain: challenges and assessment strategies. J Gerontol Nurs. 2002;28(1):20-27. 12. Collett B, et al. The assessment of pain in older people. Clin Med. 2007;7(5):496-500. 13. American Geriatrics Society Panel on Pharmacological Management of Persistent Pain in Older Persons. Pharmacological management of persistent pain in older persons. J Am Geriatr Soc. 2009;57(8):1331-1346. 14. Hager K, Brockopp D. The use of a chronic pain diary in older people. Br J Nurs. 2009;18(8):490-494. 15. Cancer pain relief and palliative care. Report of a WHO expert committee. World Health Organ Tech Rep Ser. 1990;804:1-75. 16. Chou R, et al; American Pain Society-American Academy of Pain Medicine Opioids Guidelines Panel. Clinical guidelines for the use of chronic opioid therapy in chronic noncancer pain. J Pain. 2009;10(2):113-130. 17. D'Arcy Y. Treating pain in addicted patients: great challenge, greater reward. Adv Nurse Pract. 2010;18(5):20-24. 18. Pergolizzi J, et al. Opioids and the management of chronic severe pain in the elderly: consensus statement of an international expert panel with focus on the six clinically most often used World Health Organization step III opioids (buprenorphine, fentanyl, hydromorphone, methadone, morphine, oxycodone). Pain Pract. 2008;8(4):287-313. 19. Auret K, Schug SA. Underutilisation of opioids in elderly patients with chronic pain: Approaches to correcting the problem. Drugs Aging. 2005:22(8):641-654 20. Brookoff D. Neurophysiological underpinnings of electronic analgesia neuro-modulation for dummies. Pain Medicine 2006; 7: S103-S120 21. Alberts A. Johnson A. Lewis J. Raff M. Roberts K. Walter P. Ion Channels and the electrical properties of membranes in: Molecular Biology of the Cell; 4th Edition, Garland Science, Oxford, UK, 2003, pp. 831-906 22. Savery S, Ortiz A, May H. Clinical Applications and Electro medical Treatment on Diabetic Neuropathy and Gangrene of the Toe. Advances in Therapy 1990:7:283-288 23. Becker R. Seldon G. The Body Electric; Electromagnetism and the Foundation of Life. William Morrow and Co. Inc., New York, 1985. 24. Chronic Pain Fuels Boom in Opioids - John Fauber, Reporter, Milwaukee Journal Sentinel/Med Page Today pub. Feb 19, 2012 |
|
|
|
|
|
I have had torn cartilage in my left knee since I was 19 years old. I am now 55. It's given me more or less problems over the years and I have always stayed fairly active, (I golf and ski) but I could never do anything that involved running. After 1 treatment on Saturday, I ran and wlalked the 10K in one hundred and ten minutes My knee doesn't hurt at all when as previously I would have been in extreme pain for days if I had done a tenth of that much running. This is the most amazing thing I have ever experienced" - Jerry Pool, US - - See live video testimonials at the following link: https://www.avazziatraining.com/site/page/view/testimonials/ |
1500 people gathered in Irvine Ca. to hear about this amazing technology at the T. Harv Eker Extreme Health Seminar. A dozen people were chosen at random, treated and marched back onto the stage. This is their unedited testimonial
Brian Vankirk is a train engineer who suffered from chronic damage to his knees after falling 30 feet onto metal railway ties. The medical solution was a knee replacement until he discovered this.
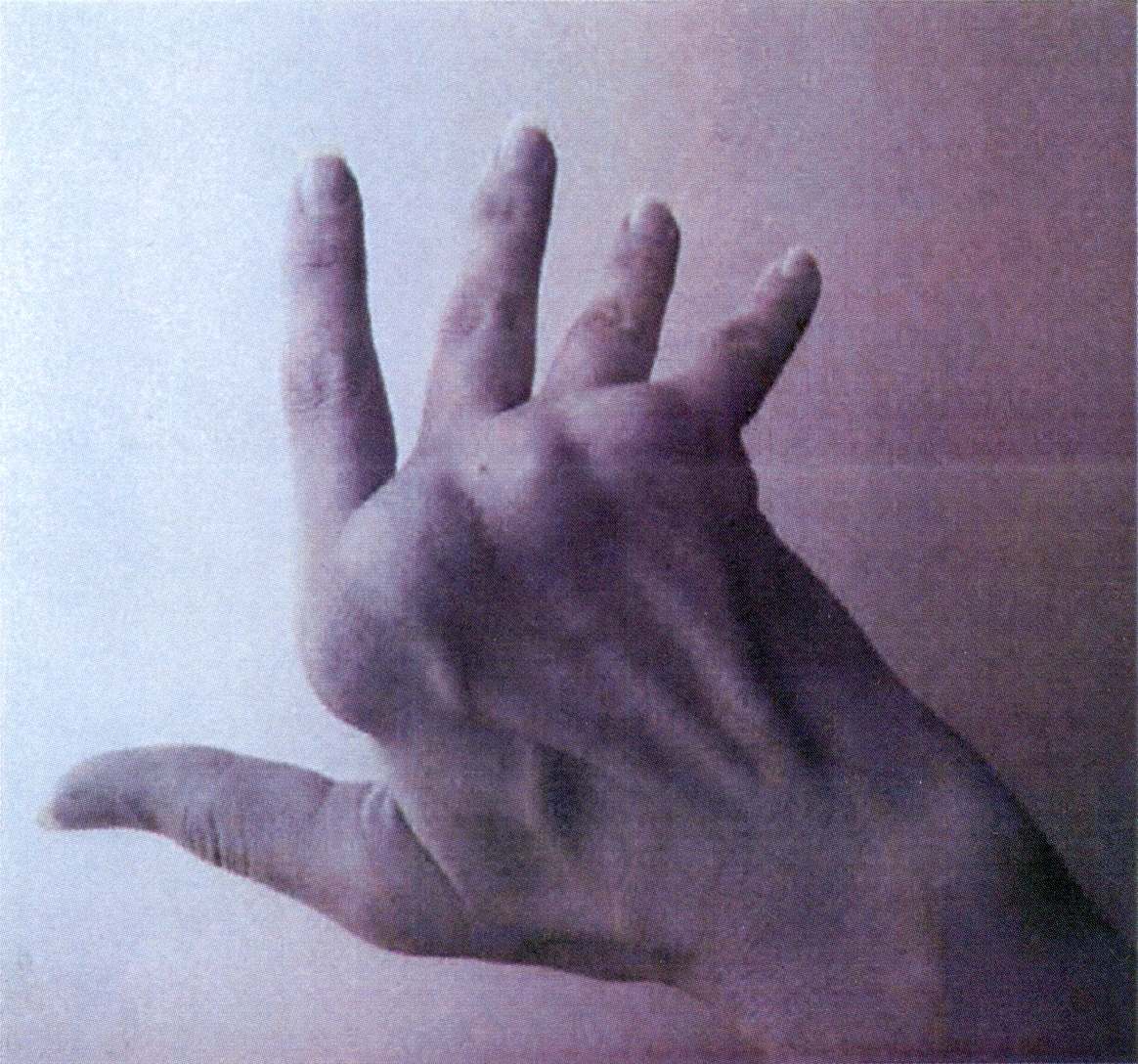
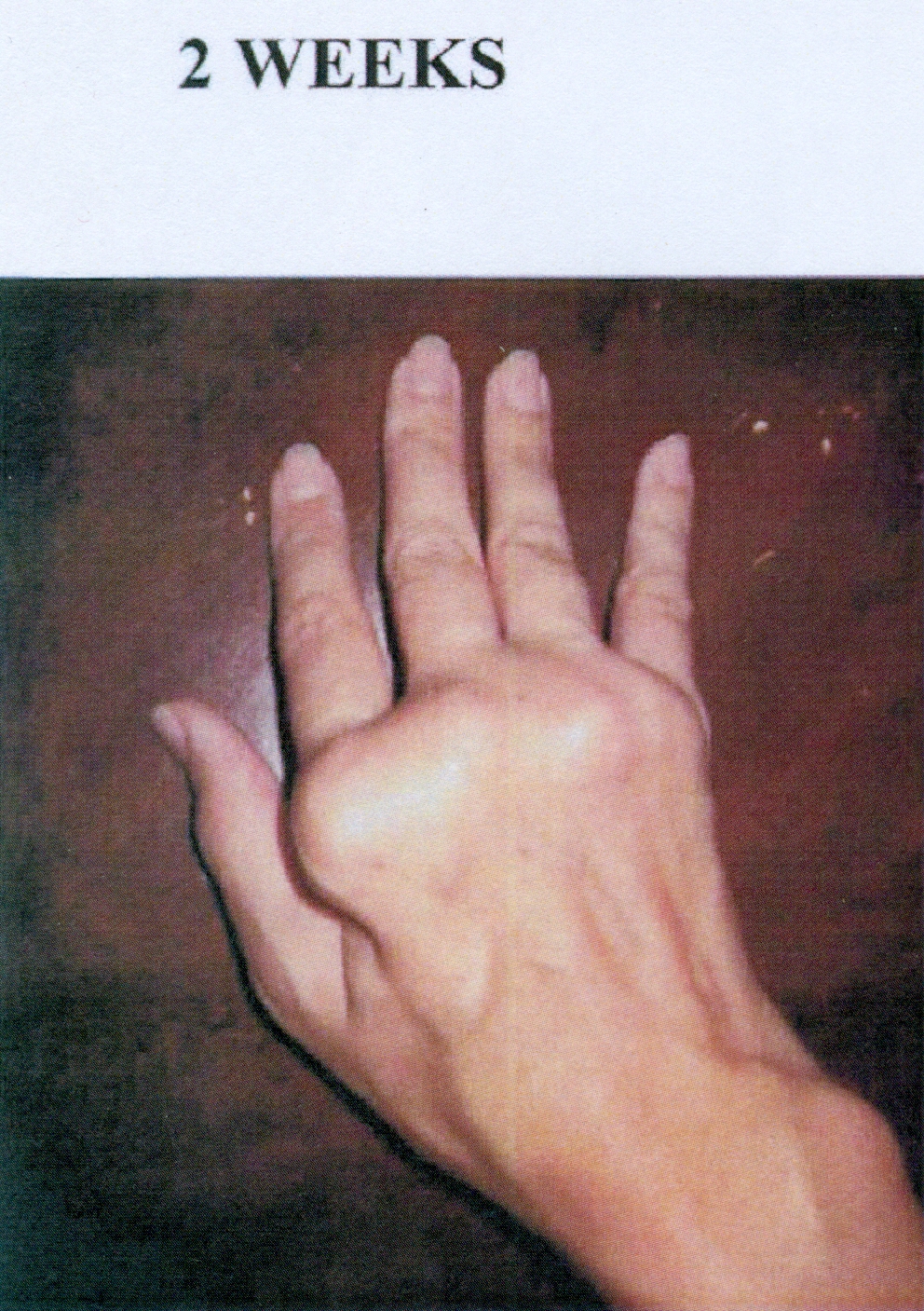
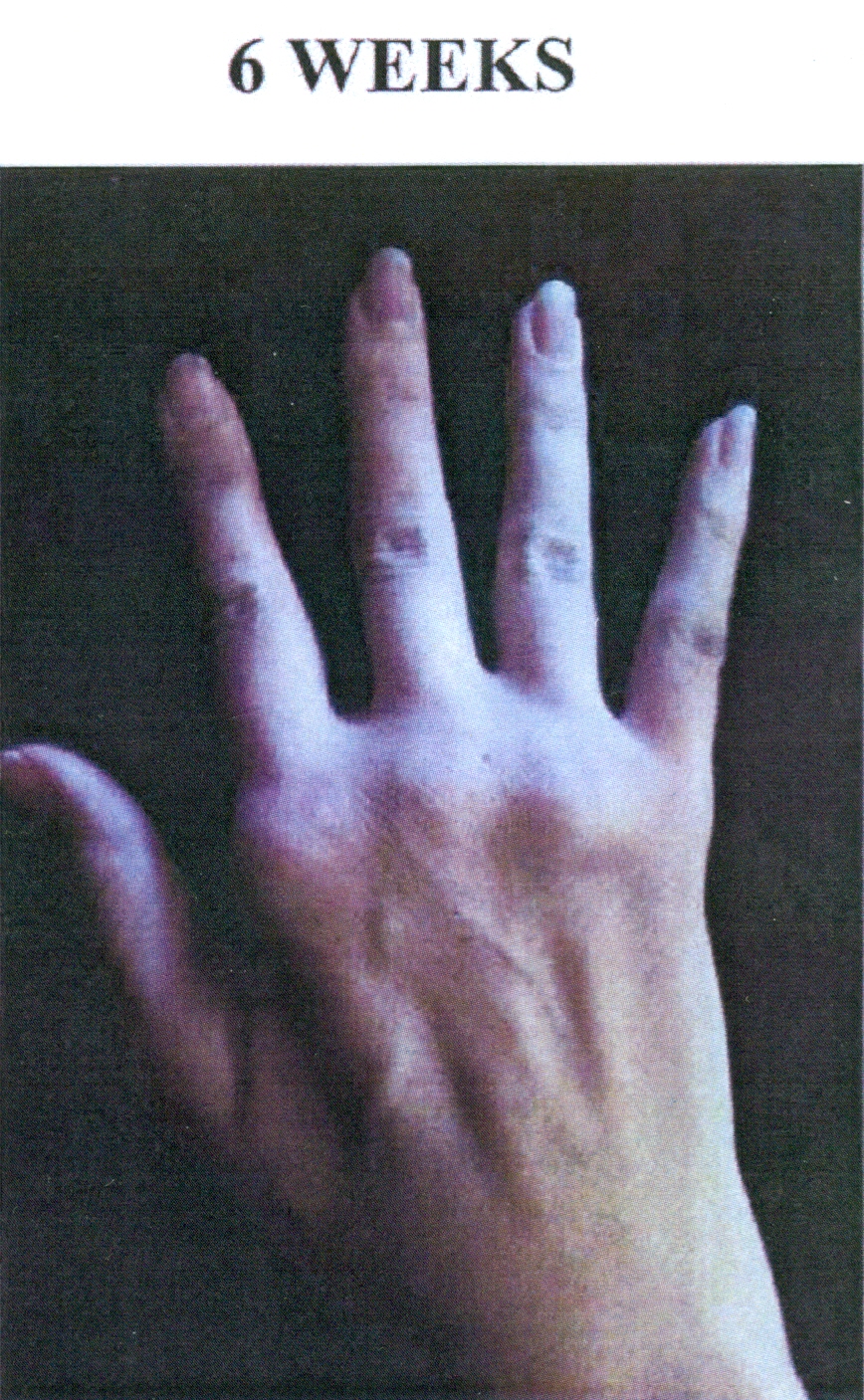
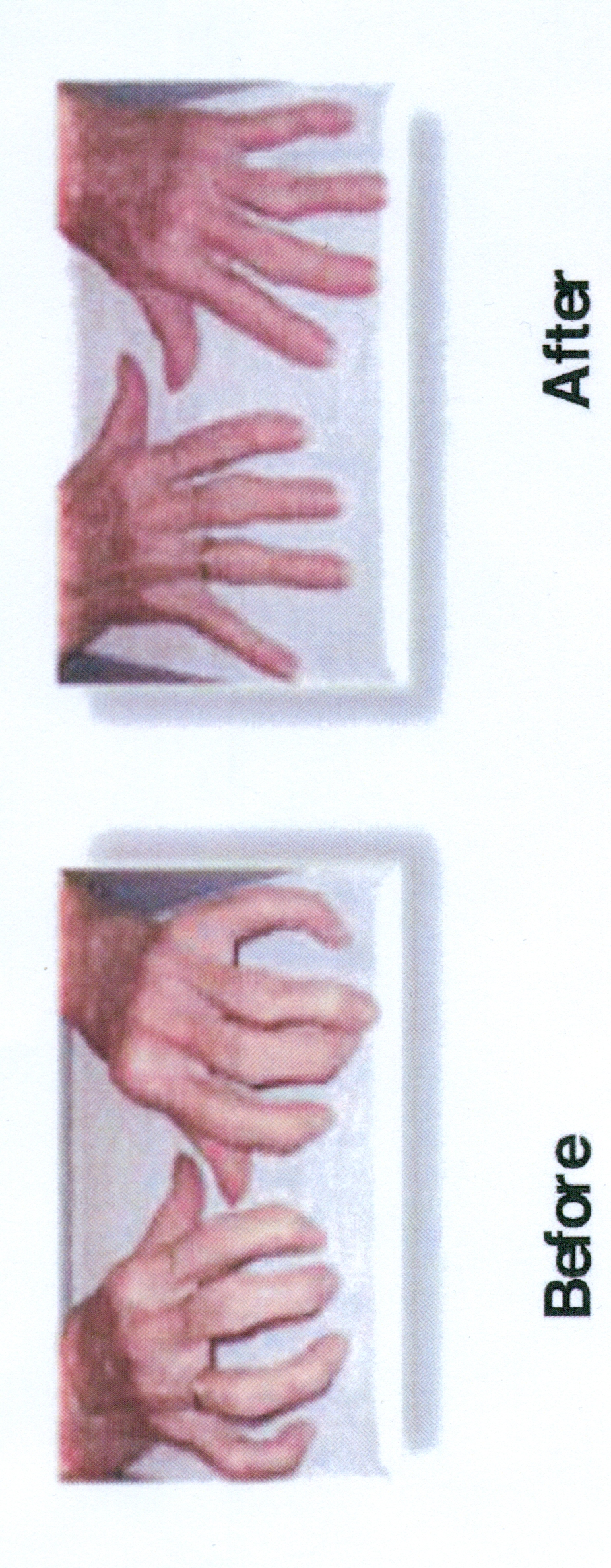
Is it possible to reverse the damage done by Rheumatoid Arthritis? The following pictures confirm that "Yes" it is possible, even after years of damage.